Fertility
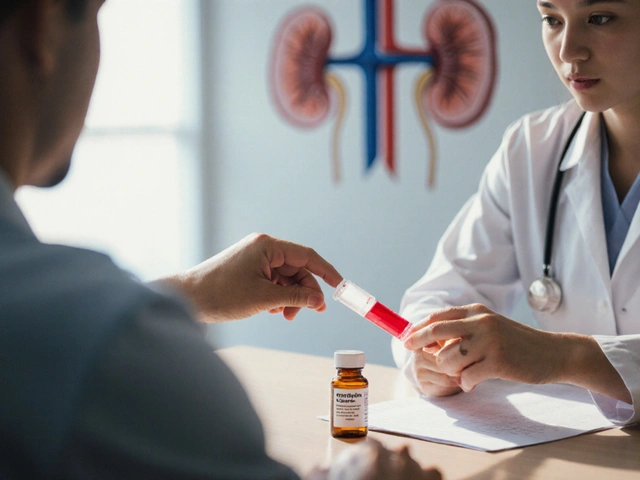
When talking about fertility, the natural ability to conceive and carry a pregnancy. Also known as reproductive potential, it hinges on a delicate balance of hormones, healthy tissues, and lifestyle factors. One of the most common ways to support this balance is with clomiphene, a selective estrogen receptor modulator used to stimulate ovulation in women facing difficulty conceiving. While clomiphene can jump‑start ovulation, it also interacts with mood pathways, which is why researchers keep an eye on its possible link to postpartum depression, a mood disorder that can emerge after childbirth and affect both new mothers and fathers. Another class of drugs, the anti‑androgens such as flutamide, can shift hormone levels enough to impact sperm production, showing how medication choice directly influences fertility outcomes.
How Hormone Therapy Shapes Your Chances
Hormone therapy is the backbone of most fertility interventions. By tweaking estrogen, progesterone, or testosterone levels, doctors can correct underlying imbalances that block conception. For example, a low‑dose estrogen supplement may prepare the uterine lining, while a progesterone boost can sustain early pregnancy. The same principle applies to men: anti‑androgens reduce excess male hormones that might harm sperm quality, but they must be used carefully to avoid suppressing fertility altogether. Understanding these trade‑offs helps patients decide when to start, pause, or switch treatments. It also explains why many people consult both a reproductive endocrinologist and a mental‑health professional—hormone shifts can affect mood, energy, and stress, all of which feed back into reproductive health.
Beyond prescription meds, lifestyle tweaks can tip the scales. Regular exercise improves insulin sensitivity, which in turn stabilizes hormone production. A balanced diet rich in omega‑3 fatty acids supports egg quality and sperm motility. Even sleep patterns matter; poor sleep spikes cortisol, a stress hormone that can suppress the reproductive axis. When these non‑pharmacologic steps are combined with targeted drugs like clomiphene or carefully monitored anti‑androgen therapy, the success rate for natural conception climbs noticeably. Patients often report feeling more in control when they see how each habit contributes to the bigger picture of fertility.
One frequently overlooked piece is the emotional side of trying to conceive. The pressure to get pregnant can magnify anxiety, and if a medication such as clomiphene alters serotonin pathways, the risk of mood swings or postpartum depression rises. Mental‑health screening before and during treatment is becoming standard practice, ensuring that any depressive symptoms are caught early and managed alongside the fertility plan. This integrated approach—medication, hormone balance, lifestyle, and mental health—creates a more resilient path to pregnancy.
Below, you’ll find a curated set of articles that break down each of these aspects in plain language. From comparing anti‑androgen options to understanding how mindfulness can calm tremors that interfere with daily life, the collection gives you actionable tips and evidence‑backed data to navigate your fertility journey with confidence.
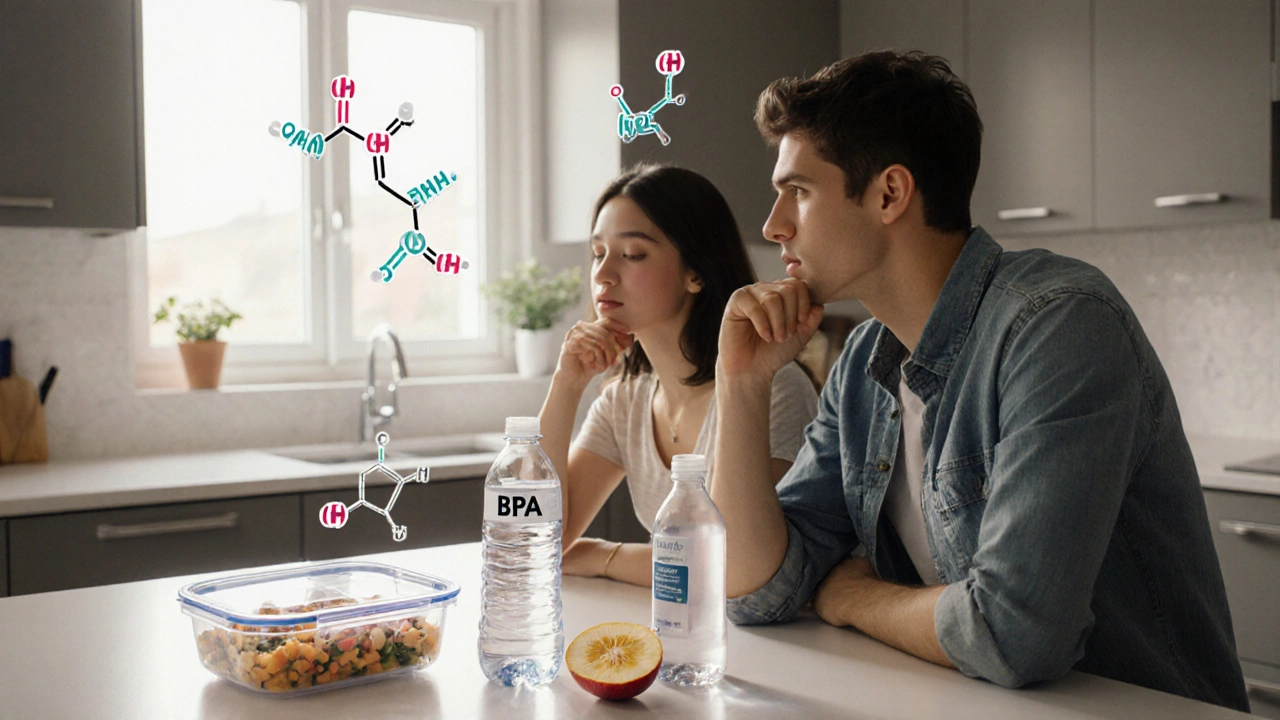
Fertility and Chemical Exposure: Key Risks to Avoid
- Date: 13 Oct 2025
- Categories:
- Author: David Griffiths
Learn which everyday chemicals harm fertility, how they affect reproductive health, and practical steps to avoid exposure for a healthier conception journey.